Introduction
The global Covid-19 crisis will lead to unprecedented change. Certain healthcare sectors will be re-defined as strategic infrastructure and new trends will emerge that will persist beyond the crisis. In this paper we examine the five key post-Covid-19 trends and the likely investment opportunities that will arise.
Download white paper
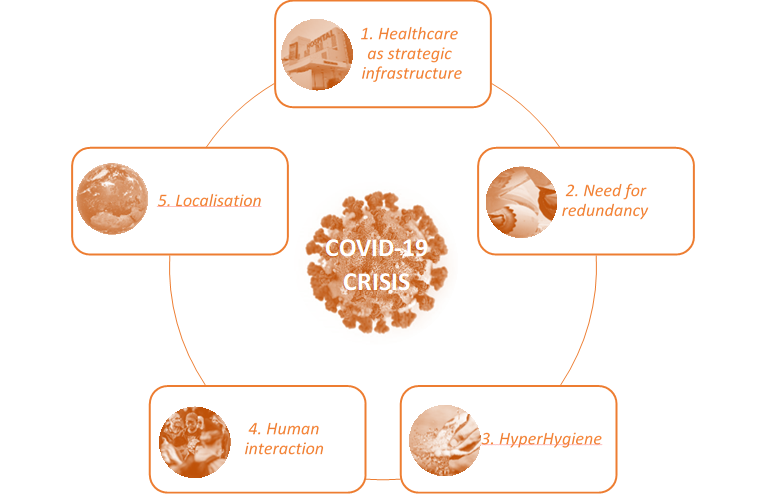
Key Trends

1. Healthcare as strategic infrastructure
For decades, healthcare has been perceived as a cost to be managed through multiple tools like access, utilization and pricing. This crisis will cause us to reconsider healthcare as a strategic infrastructure that not only shields us from future pandemics but protects economies and confers a competitive advantage at a regional and national level. As healthcare systems invest in the new healthcare infrastructure, there is a unique opportunity to overcome some of the historical obstacles (e.g. legacy infrastructure, medical education) and embrace change.
Impact: New healthcare infrastructure such as alternate care sites and channels (e.g. telemedicine, care-at-home), and disruptive technologies (e.g. AI-driven care, virtual trials).

2. Need for redundancy
Many countries have optimised their healthcare capacity and stocks in a drive towards containing cost and maximizing efficiency. The Covid-19 crisis has evidenced the need for increased redundancy in healthcare systems to cope with shocks. However, the traditional approach of surplus capacity and large inventories is prohibitively expensive.
Impact: New models will be sought to provide for fungible, agile infrastructure and systems that enable rapid transformation of healthcare capacity to address emerging crises (e.g. temporary facilities as mobile health infrastructure that can be rapidly transported and deployed, flexibility in factory lines allowing switching to the production of essential equipment).

3. HyperHygiene
Healthcare providers, patients, and consumers will demand different habits and a new level of hygiene and health certification. In particular, as more care localises (see “localisation” trend) the new hygiene standard will extend from hospitals and care homes, via travel through airports and railway stations, all the way into daily life in shops, restaurants and the home.
Impact: Supply chains, product and packaging certifications will need to be reimagined to extend the new hygiene standard all the way into the home. Public transport will have to be made safe, people may have to carry health certificates to gain access to certain spaces and services.

3. Human Interaction
Long-term or recurrent social distancing may be required but is incompatible with the current ways of delivering healthcare or indeed normal daily life. A “touchless” ecosystem will evolve permanently altering human interaction, including social and generational distancing. Private home solutions will be preferred over unnecessary exposure to groups. One of the major side-effects will be more anxiety, loneliness and depression, especially in the already vulnerable elderly.
Impact: The trend towards remote delivery of health care will accelerate.Alternate care sites will emerge with a shift towards the home (remote mental care, home therapy, home monitoring/testing/certification, eDetailing). Public interfaces will become touchless (e.g. cash or ticket machines, traffic light switches).
5. Localisation
Complex global structures have not aided the response to the Covid-19 crisis in e.g. taking swabs and running SARS-CoV2 tests or the provision of essential PPE and medicines. The new trend in localisation will focus on control and access during potential crises (moving global to regional, national or local) and will accelerate especially as healthcare is recognized as strategic infrastructure. Some areas that have globalised will localise for strategic and health security reasons and the key will be preserving the benefits of scale and accumulated experience in the local setting.
Impact: Generics, PPE and other manufacturing and supply chains (e.g. certain diagnostics) will localise.
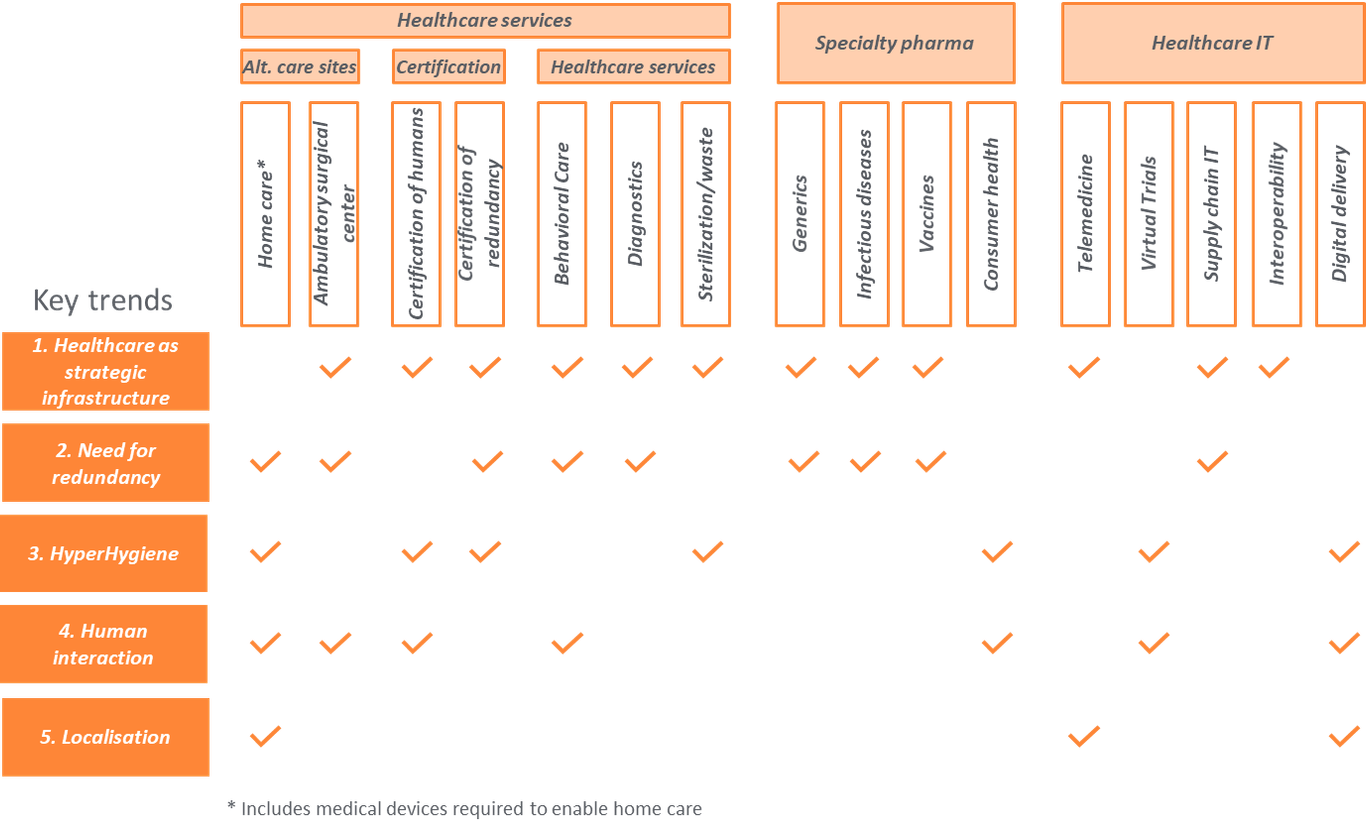
Impact by sector
Sectors are impacted by multiple trends. In this table, we identify the sectors that will be impacted and where we believe there are investable theses:

Key Takeaways
The Covid-19 crisis will re-define certain healthcare sectors as strategic infrastructure and result in permanent change driven by the trends discussed here. As a result, we expect an acceleration of the overall healthcare expenditure due to the need to invest in strategic infrastructure and new business segments in the post-Covid-19 world. We believe new and attractive investment opportunities will emerge in both strategic infrastructure and new business segments. Investors who can access deep experience and specialization in healthcare will be well positioned to take advantage of these opportunities.
© 2019
All Rights Reserved

